Introduction
Mupirocin ointment is a topical antibiotic approved for the treatment of cutaneous staphylococcal and streptococcal infections [1]. Despite its side effects, which include mild burning sensations and pain, mupirocin has been reported to be safe and well tolerated and is known to cause allergies in only extremely rare cases. To date, a small number of cases of mupirocin-induced contact allergic dermatitis have been noted [1-3]. We report a rare case of severe allergic contact dermatitis resulting from treatment with mupirocin ointment. Written informed consent to publish case details was obtained from the patient.
Case
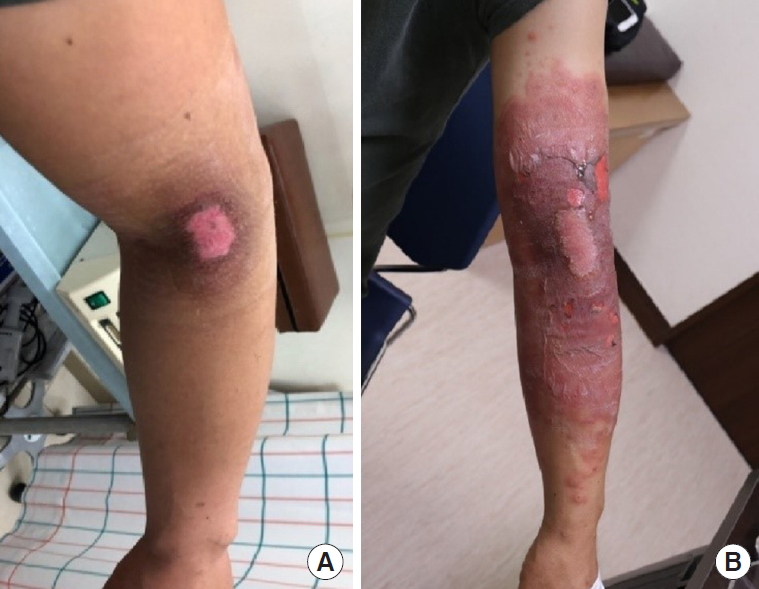
A 41-year-old male patient without any allergic history visited our hospital after sustaining a chemical burn on his left elbow from contact with an unknown acid. At that time, the wound was limited to the elbow area, was 4×4 cm in size, and appeared to be an erythematous lesion with minimal ruptured bullae (Fig. 1). To prevent wound infection and to provide moisture, mupirocin ointment (Esroban Oint; JW Shinyak, Seoul, Korea) and a foam dressing (MediTouch; Ildong Pharmaceutical Co., Ltd., Seoul, Korea) were applied daily while for parts of the wound with first-degree chemical burns, only the mupirocin ointment was used.
After 2 days of treatment, the patient experienced an itching sensation, and a cutaneous erosive lesion gradually spread around the initial wound. As the wound exacerbation was considered a result of aggravation of the chemical burn, the method of dressing was maintained under observation. However, on the 3rd day of treatment an exfoliative skin lesion and bullae formation appeared where the mupirocin ointment had been applied, and this lesion quickly spread to the entire left upper extremity (Fig. 1). Because the patient had a history of several treatments with same foam materials in simple wounds, and also because the allergic reaction spread beyond the area where foam materials had been applied, the diagnosis was a severe allergic contact dermatitis to mupirocin ointment rather than an allergic reaction to foam materials. The use of mupirocin was terminated, and the spreading and aggravated erosive cutaneous lesion was treated with normal saline and wet-gauze dressing. Additionally, to subside the itching sensation during treatment, an antihistamine was prescribed. In consideration of the adverse effects of topical or oral steroids such as delayed re-epithelization and wound healing, no steroid cream was used. After the use of mupirocin was discontinued, there was notable improvement of pruritis and reduced expansion of the wound.
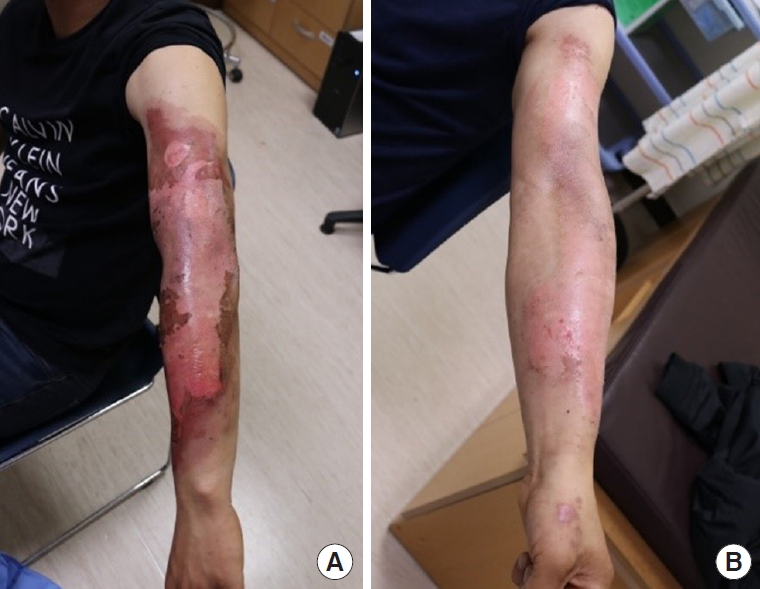
One week after changing the dressing method, most of the erosive lesion had started to re-epithelize, and after 2 more weeks, there was full epithelization and the wound had completely healed (Fig. 2). Our clinical diagnosis of this rare case was severe allergic contact dermatitis caused by mupirocin ointment.
Discussion
Mupirocin ointment is used as a topical antibiotic worldwide to treat or prevent staphylococcal and streptococcal infections. Its active ingredient was extracted from Pseudomonas fluorescens in 1971 [1,4]. Mupirocin reversibly binds to bacterial isoleucyl-transfer RNA synthetase and thereby suppresses bacterial protein and RNA production in cutaneous infectious lesions [5].
Because mupirocin is effective for treating most cases of cutaneous infection, it has been used in a variety of wounds. This drug is particularly useful for treating both primary and secondary superficial skin infections caused by Staphylococcus aureus isolates (such as furuncle, impetigo, surgical wounds), usually with 80% improvement in infected patients and 90% eradication in the S. aureus isolates. Furthermore, mupirocin ointment is applied to wounds associated with cutaneous defects to prevent cutaneous infections and to provide a moist, sterile environment that facilitates optimal healing [6].
In most cases, when this ointment is applied to wounds, the only side effects and cutaneous symptoms are a temporary burning sensation or pain, observed in less than 3% of patients. With only rare reports of contact allergic reaction to mupirocin, there were no known cases of systemic side effects that were severe enough to evoke anaphylaxis or diarrhea [7].
In our case, because the elbow wound was caused by a chemical burn from an unknown acid, we expected that it might exacerbate but only in the initial wound area. However, after applying mupirocin ointment to the wound, aggravated cutaneous symptoms, including bullae formation, skin exfoliation and pruritis, were observed over the treated area. Initially, these intensified symptoms were regarded as a manifestation of the natural course of the chemical burn instead of a rare allergic reaction to mupirocin, and as a result, lesions severely worsened and spread to the entire left upper extremity.
As mentioned above, very few cases of mupirocin contact allergic dermatitis or reaction have been reported [1-3], and no case of severe allergic reaction to mupirocin has been described. Because such cases are largely unheard of, surgeons or physicians unaware of the association between mupirocin and allergic reactions are likely to be confounded when they encounter such a case. We hope our report will raise awareness on this rare situation and enable proper decision-making to prevent exacerbation or spread of the wound.
In conclusion, allergic reaction or dermatitis resulting from mupirocin ointment is rarely reported. When a surgeon or physician encounters a situation similar to this rare case, hopefully our report will help them make correct diagnoses and decisions to prevent the wound from worsening or spreading.