Introduction
Penile defects have a variety of causes including traumatic, idiopathic, or iatrogenic events. Among them, iatrogenic causes include corrective surgery for urethral fistula or penile deviation, foreign body reactions caused by substances inserted for penile augmentation, and necrosis after congestion caused by overuse of Viagra [1]. Some defects resulted from infections of the perineum or scrotum, such as Fournier gangrene. Such infections of skin and soft tissue can cause necrosis and defects in the perineal region [2,3].
Multiple methods have been proposed to reconstruct penile defects of different origins, and each has its strengths and weaknesses. Skin graft reconstruction is the simplest, but it is not able to secure appropriate volumes and has the associated risk of shearing and contracture [4,5]. The scrotal flap technique is simple with fewer complications, but it is difficult to obtain appropriate bulkiness, and has cosmetic disadvantages after surgery arising from ectopic hair growth [6,7]. The radial forearm free flap provides an adequately thin flap and yields good results in terms of appearance and function, but requires a microscopic procedure and has relatively high complication and donor morbidity rates [8]. On the other hand, the groin flap, while often requiring two-stage surgeries, yields better erectile function and penile bulkiness to fill the contour defect than the skin graft technique and also requires a shorter operation and results in fewer complications than other flap methods [5]. Here, we describe six cases of penile defects treated with reconstructive surgery using groin flaps.
Methods
We performed a retrospective chart review of patients with penile defects treated in our department between March 2009 and September 2013. The study was performed in accordance with the principles of the Declaration of Helsinki. All patients provided written informed consent for the publication and the use of their images.
After proper pretreatment, including dressing and debridement of necrotic tissue, all patients underwent reconstruction surgeries using a groin flap. Before the surgery, we took a digital photo of the defect area using a paper ruler as a scale. We analyzed the photo using ImageJ software (National institute of Health, Bethesda, MD, USA) and measured the area of the defect.
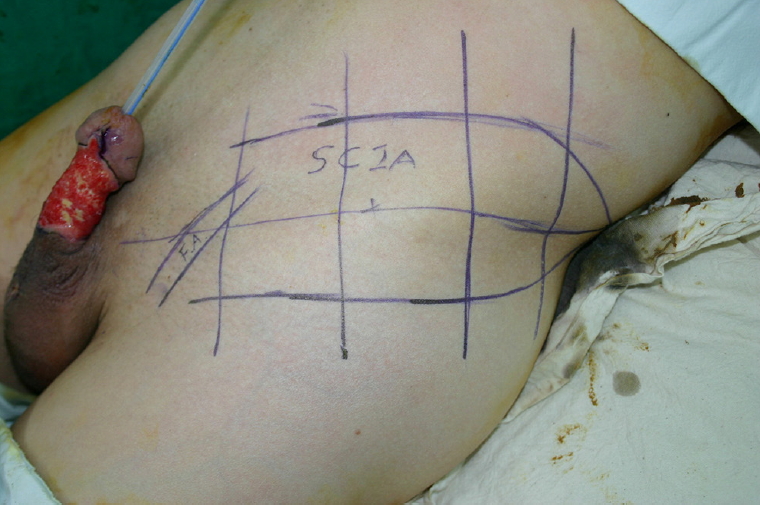
All patients had surgery under general anesthesia in a supine position. To minimize damage of the dorsal neurovascular bundle, all inflammatory tissues including necrosis were removed above Buck’s fascia. For the first stage of operation, a flap pattern was drawn on the groin after marking the direction of blood flow of the superficial circumflex iliac artery using a Doppler ultrasound device. Depending on the defect size, a flap of width from 6 to 8 cm was designed so that its major axis was parallel to the inguinal ligament (Fig. 1). Dissection and flap elevation were carried out from anterior superior iliac spine (ASIS) aspect to pubic tubercle aspect along the major axis of superficial circumflex iliac artery and venae comitantes (i.e., dominant pedicles running parallel about 3 cm below the inguinal ligament in the flap), and the superficial circumflex iliac vein. Initially, dissection was carried out above the deep fascia, and the flap was dissected below the fascia when it reached the sartorius muscle after passing the ASIS in order to avoid damaging the superficial circumflex iliac artery. As the dissection takes place, the superficial circumflex iliac vessels can usually be visualized on the under surface of the fascia. After exposing the vascular pedicle, the dissection was carried across the floor of the femoral triangle to the lateral edge of the femoral sheath to identify the origin of the superficial circumflex iliac artery from the femoral artery. The elevated flap was then rotated, exposing the flap pedicle, and moved to the defect area without any strain in order to conduct annular coverage of the penile defect.
The thin portion of the flap elevated in the lateral area of the sartorius muscle was used to cover the penile defect by winding around the penile shaft. Meanwhile, the medial and relatively thick portion of the flap that includes deep fascia was mainly used to cover the scrotal defect to provide adequate volume for the defect area and to protect the testis. In cases where there are few or no scrotal defects and an inner flap is not required, a medial thick portion of the flap was resected during the second stage operation.
In a patient with a urethra defect, the defect was reconstructed using a full-thickness skin graft (FTSG), because the width of the donor site did not exceed 8 cm, and direct closure of donor site was conducted with the thigh bent. The second stage operation for pedicle division and flap contouring was performed under local anesthesia 3 weeks after the first stage operation.
However, if there is a skin and soft tissue defect limited to the caudal or lateral portion of the penile shaft, (i.e., not a defect on the entire circumference of penile skin), and the defect area does not extend to the proximal part of the elevated groin flap, there is no need for annular coverage of the penile shaft. In this case, we preserved the intact skin and soft tissue of cephalic penile shaft area, and a single-staged coverage was performed using a groin flap as a local pedicled transposition flap.
Duration of operation and recovery periods, and postoperative complications were compared through a chart review. Duration of operation refers to the total amount of time required to perform the operation. Recovery period refers to the period from the date of the first stage operation to the time of discharge after the second stage operation. Bulkiness comparisons were conducted by measuring the circumferences of the middle portions of resting penile shafts at 1 and 10 months after surgery. Voiding difficulties and erectile pain and dysfunction were noted.
Results
Clinical analysis of patients
The causes of the defects and their locations and sizes before surgery were determined. The patients were five males and one female who had female to male gender identity disorder with ages ranging from 30 to 59 years (mean, 40.83 years). The causes of the skin defects were: (1) necrosis resulting from foreign substance injection, one case by paraffin and another by silicon; (2) lasting side effects of congestive blood after taking Viagra; (3) complication after surgeries to treat hypospadia and deviated penis; and (4) complication after forearm free flap surgery for reconstruction of total phallus in the female to male gender identity disorder patient (Table 1).
Defect areas in the six patients were localized to penis and scrotum, and average defect size was 66.41 cm2 (range, 45–99 cm2). The six patients recovered after groin flap surgery without any severe complications, such as infection, flap necrosis or flap loss, and neither were any significant complications observed on the donor sites. Though minimal wound dehiscence lasting more than a week was observed in four patients after surgery, they recovered naturally within 2 weeks without special treatment. In addition, one patient with partial skin necrosis also recovered fully after a partial skin graft. In particular, the patient that underwent a urethra reconstruction operation with FTSG had no problems in voiding function. Unfortunately, most of the patients could not measure their circumference in normal condition, because they came after they had already been wounded. The circumferences of penile shafts were measured at 1 and 10 months after surgery, and resting penile shaft bulkinesses were found to be maintained at >86% (Table 2). According to literature, the average circumference of an erect human penis is 11.66 cm [9]. Although a direct comparison is not possible because we measured the resting penile circumference, the average resting circumference was 11.11 cm, slightly smaller than the average erect circumference. We therefore expect that the erection circumferences of our cases are close to the average circumference of an erect human penis.
None of the patients showed any significant complication or erectile dysfunction or pain during erection owing to defective contracture, which is a potential cause of appearance and functionality problems (Table 3). Follow-up periods after surgery ranged from 10 to 25 months (mean, 16.16 months), and natural penile shapes were maintained at last follow-up with normal urination and erection (Figs. 2-4).
Case presentations
Case 1
A 34-year-old man was treated with silicone injection for penile augmentation 4 years previously. He visited us 2 weeks prior to surgery complaining of penile pain, inflammation, and discharge. He had previously sought treatment for his symptoms at a local medical center, but his condition did not improve. The patient received debridement and foreign body removal treatment. The two-stage groin flap surgery was initiated after infection and inflammation were controlled by daily dressing and anti-biotics treatment. At the first stage surgery, the flap was elevated from the left groin area to cover the defect on the penile shaft. Flap division was conducted 3 weeks after the first stage surgery. The patient recovered without significant complications. After flap division surgery, the patient’s genitals had an acceptable cosmetic appearance and the bulkiness of penile shaft was maintained at 92% after 10 months of surgery. No significant complications were identified after the surgery, and erectile and voiding function were well maintained (Fig. 2).
Case 2
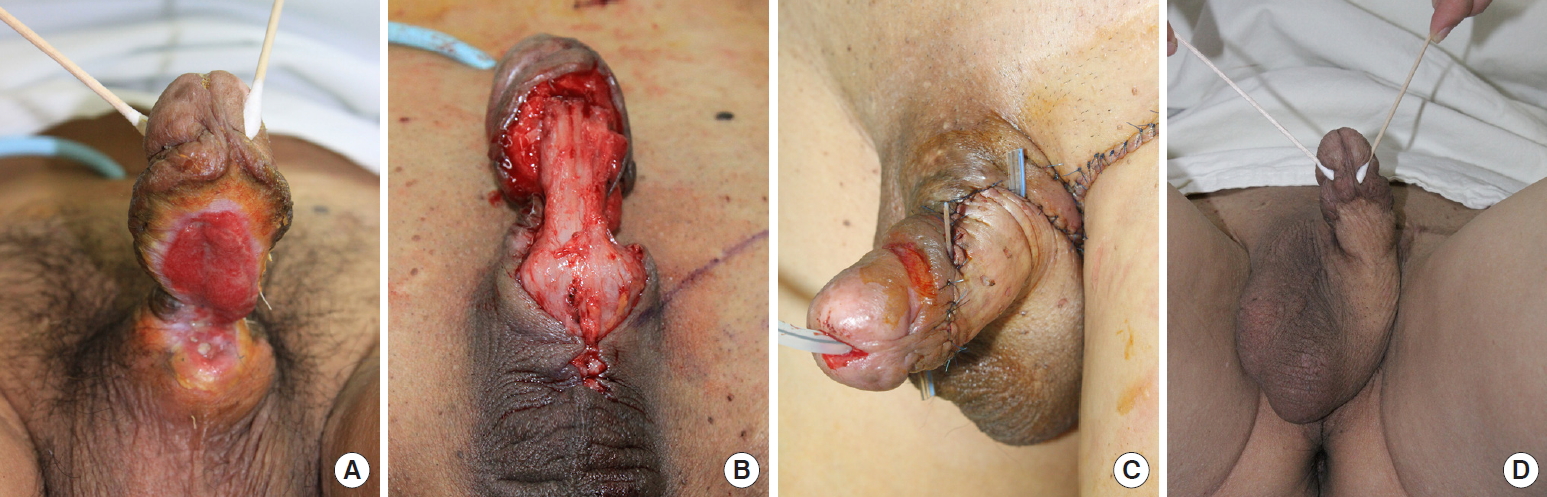
A 59-year-old man suffered from penile necrosis due to sustained erection and congestion after taking illegal anti-impotence drugs 10 days previously. He visited us for treatment of the penile skin and soft tissue defect after debridement of necrotic tissue at a local medical center. After debridement of unhealthy tissues, the extent of the defect was limited to the left lateral, caudal part of penile shaft and small upper scrotal area. Single-stage groin flap surgery was carried out using a pedicled local transposition flap. He fully recovered without significant complications, and postoperative appearance was satisfactory. Resting penile bulkiness was maintained 94% at 1 and 10 months after surgery, and erectile and voiding functions were well maintained (Fig. 3).
Case 3
A 31-year-old man visited us for penile reconstruction. He had suffered partial penile skin and soft tissue loss due to penile necrosis after undergoing surgery to correct penile deviation. A groin flap was elevated from the left inguinal area, and penile shaft reconstruction was performed with a tubed groin flap. The damaged urethra was reconstructed using FTSG with skin harvested from right inguinal area. Afterwards direct closure of both inguinal donor sites was performed. Three weeks later, seeing the flap well engrafted and surviving, we performed the separation and contouring operation. The patient recovered fully without significant complications and expressed postoperative satisfaction. The resting penile bulkiness was maintained at 94% between 1 and 10 months after surgery, and erectile and voiding functions were also well maintained (Fig. 4).
Discussion
Among the diverse etiologies of penile skin and soft tissue defects, there has been a recent increase in defects resulting from necrosis after conducting various procedures for penile augmentation [10,11]. Fat injection is frequently used for penile augmentation, and in some cases, foreign material including silicone, paraffin, or oil are injected by non-practitioners. In such situations foreign body reactions are likely to incur inflammation and infection, and sometimes vascular embolization may even lead to necrosis. Necrosis can also be caused by other treatments, such as suspensory ligament release using a V-Y advancement flap to lengthen the shaft, or by complications after surgeries to correct penile deviation or urethral fistula [12]. In some cases, defects are generated by extensive resection of a perineal tumor, extramammary Paget disease, or Fournier disease.
Despite the availability of many reconstruction techniques, no clear guidelines have been established regarding optimal reconstruction techniques. Ideally, procedures should be safe and relatively easy to perform and free of risk of complications at defect and donor sites. The purposes of the reconstruction are: (1) to obtain a natural appearance with minimal donor site scarring; (2) to ensure comfortable urination with normal function; and (3) to ensure conditions enabling sexual intercourse [13]. Currently, the reconstruction techniques used are skin grafts or scrotal, anterolateral thigh (ALT), groin, pudendal artery perforator flaps, etc.
Because it is a simple, safe technique without serious complications, the skin graft technique has been widely used. However, the method may cause depression deformation if too much subcutaneous fat is removed and it also presents a high risk of scar contracture that might result in functional and cosmetic issues. Contracture of grafted skin causes erectile dysfunction and or pain during erection [14-16].
Several techniques using the scrotal flap, such as the Ceciltype scrotal flap, have been introduced, whereby the scrotal branching of the lower pudendal artery is taken as the base. The technique implants the denuded penis below the skin of the scrotum for 2 to 4 months when the scrotum skin is used to cover the skin defect. This method is advantageous because it has low risk of necrosis and contracture, but it requires a secondary operation and may result in urethral damage. Although the bilateral scrotal flap technique, which is a modification of the Cecil-type flap, does not have the shortcomings of other techniques, the suture line is located on the dorsal penis, and the wound is visible during urination. In addition, blood vessels may be damaged while elevating the scrotal flap and skin contracture can occur on the dorsal and ventral penis upon erection. Z-plasty can be used to address these problems, but the risk of flap necrosis remains. Although the scrotal flap technique has low donor site morbidity, this technique has the drawback of ectopic hair growth arising from the wrinkled hairy scrotal skin that was transferred to the penile shaft, in addition to the above-mentioned cosmetic problem [7].
The ALT flap has a long vascular pedicle, and accordingly, is suitable for the reconstruction in the suprapubic region and is good for thickness adjustment. However, it has the shortcoming of larger scars on the donor site. Because the ALT flap is located at a distance from the perineum, this method is only possible if an ALT pedicle that enables moving the flap to the penoscrotal defect area is identified. While in most cases, primary closure of the donor area is possible, for wider ALT flaps, a skin graft is required for closure of donor area. For these reasons the morbidity rates of the donor site are higher, and the ALT flap is generally not favored as a surgical method [4].
Using the pudendal artery perforator flap is a preferred method of operation for perineal reconstruction. The thickness of superficial external pudendal artery (SEPA) perforator flap is measured at 3 to 10 mm. Because this method allows for thin covering, SEPA perforator flaps are used in cases where thin flaps are important, such as penile shaft reconstruction. However, as SEPA perforator flaps are limited in the length of the pedicle, the surgical technique may be unsuitable for large defects or large penises [17].
The internal pudendal artery perforator flaps are good for coverage of scrotal area defects, and for disguising the donor site within a gluteal fold. However, the location of the flap pedicle makes it difficult to reconstruct a penile shaft defect. In this case, other surgical techniques like skin grafting may be necessary to cover the penile shaft defect [4].
When the thigh or lower abdomen is used as the donor site, axial skin-fat flaps based on the superficial epigastric artery or pudendal artery and tensor fascia lata musculocutaneous flap can easily transplant tissues containing abundant blood vessels to defect sites without requiring microscope anastomoses. However, this flap is very thick, and cosmetic and functional problems may arise from the larger amount of subcutaneous fat the flap contains [18,19].
The free radial forearm flap can be prepared as a thin flap used for cases of complete penile loss, and its color matches that of the recipient site. It can also be rolled to form a urethral pipe of sufficient length and appropriate volume. However, appropriate microscopic anastomosis is required and the surgery takes a long time, while the risk of donor site scarring and possible postoperative morbidity also limits use of this method [20,21]. We performed free radial forearm flap in cases of total penile loss, such as male pseudohermaphroditism, traumatic total loss, or gender identity disorder patients.
If partial reconstruction is required, the groin flap is considered more suitable, because results are generally satisfactory both in function and appearance, and it is without risk of serious complications like total flap loss or ischemia of the hand. Groin flaps have been used extensively since McGregor and Jackson [22] described the technique for the first time in 1972. In terms of anatomy, the groin flap is a pedicle flap containing the distributed superficial circumflex iliac artery, which can be classified into the following three zones: (1) the pure axial zone from the femoral artery to the sartorius muscle; (2) the transition zone up to the region 5 cm outside the sartorius muscle; and (3) the random zone from 8 to 10 cm from the sartorius muscle [23]. Groin flaps can cover extensive defects of over 10×15 cm without sacrificing a major artery or requiring end-to-end microvascular anastomosis [24].
As a pedicle flap with abundant blood flow, the groin flap is easily converted to a cylindrical shape. Moreover, the groin flap is hairless, of sufficient size, and readily enables penile augmentation with relatively few complications. In addition, this flap can be used to treat wide defects, and its operation procedures are simpler than those required for other flaps. Furthermore, the low contracture of this flap manifests as fewer erectile problems. Primary closure of the donor site is available with few donor site complications. The donor site scar can also be covered or hidden easily with underwear [25].
When designing the flap, the inguinal ligament is palpated and marked in its course between the pubic tubercle medially and the ASIS laterally. Whenever possible, the superficial circumflex iliac artery is identified with the Doppler probe and marked. If the superficial circumflex iliac artery cannot be identified, imaginary vascular axes are marked by drawing parallel lines about 2.5 cm below the inguinal ligament. The flap should then be marked out extending toward ASIS, beginning at the projected lateral border of the sartorius and with the upper and lower borders of the flap 5 cm above and below the vessel axis. The length then can then be determined by planning backward from the defect to be covered.
Upon elevating the flap, sufficient care should be taken to not damage the lateral cutaneous nerve of the femur that passes above the sartorius muscle. If the width of flap is less than 10 cm after elevation, the donor wound generally can be directly closed. However, if the flap width exceeds 10 cm, skin graft may be necessary to cover the donor site defect [23].
In our cases, although wound dehiscence of the flap transition area were observed in four out of six patients, the size of the dehiscence was very small, and they recovered without any special treatment. We believe the reason for the dehiscence was the partial necrosis of the fat cells contained in the seroma that formed on the flap.
So far, the general view was that the groin flap is too thick to be used for the reconstruction of the penis. But as evidenced in the postoperative results of this paper, the area of the groin flap elevated in the lateral part of the sartorius muscle that does not contain the deep fascia was flexible and not thick, making it suitable for reconstruction of the penis. The authors were able to achieve excellent cosmetic and functional results with the groin flap, which is more durable and provides better volumetric results than skin grafts and is less bulky than other flap methods, with minimal donor site morbidity.
The shortcoming of the groin flap is that the pedicle is relatively short, only about 3 cm. Also, the T12 innervation is at the lateral margin of the groin flap away from the pedicle, precluding use as a sensate flap, making decrease of sensation on penile skin inevitable. Another drawback is that the skin on the flap is paler and makes for a poor match. However, it still has the advantage of less problems with ectopic hair growth, compared to a scrotal flap.
Although there are a few limitations in the pedicled groin flap, we recommend the use of the groin flap technique as a safe, simple, aesthetically acceptable and effective means of reconstructing penile skin and soft tissue defects.