Introduction
Since the beginning of the coronavirus disease 19 (COVID-19) pandemic in 2019, the clinical reality of the medical field has undergone several changes. Emergency surgery is often delayed or cancelled because of coronavirus infection. In these cases, surgical management may not be performed in a timely manner, and the patient may die or experience severe complications. There are medical institutes where emergency surgery is impossible for patients infected with COVID-19 because the operating rooms (ORs) are not equipped with negative pressure equipment. This “new normal” gives rise to the need to consider different management scheme for the COVID-19 era.
Intravenous regional anesthesia (IVRA), also known as Bier’s block, was first described in 1908 by the German surgeon August Bier [1]. This method is a simple way to anesthetize the upper extremities using minimal equipment. With recent improvements in facilities, equipment, and manpower, most upper extremity surgeries are performed using a brachial plexus block; therefore, Bier’s block is not widely used nowadays [2]. However, the simplicity and safety of IVRA for extremity anesthesia has not changed. Furthermore, it does not require meticulous technique. This method is suitable for use in isolation rooms where space and manpower are limited.
Here, we describe three cases of emergency surgery for COVID-19 patients with upper extremity arterial injury. Since these patients were not allowed to enter the OR due to hospital rules, surgery was done under IVRA performed by the operating surgeon in an isolation room without an anesthesiologist. The report was approved by the Institutional Review Board of Dongguk University Hospital (IRB No. 110757-202211-HR-03-02). The patients were informed that this case study would be submitted for publication and provided written informed consent.
Case
Case 1
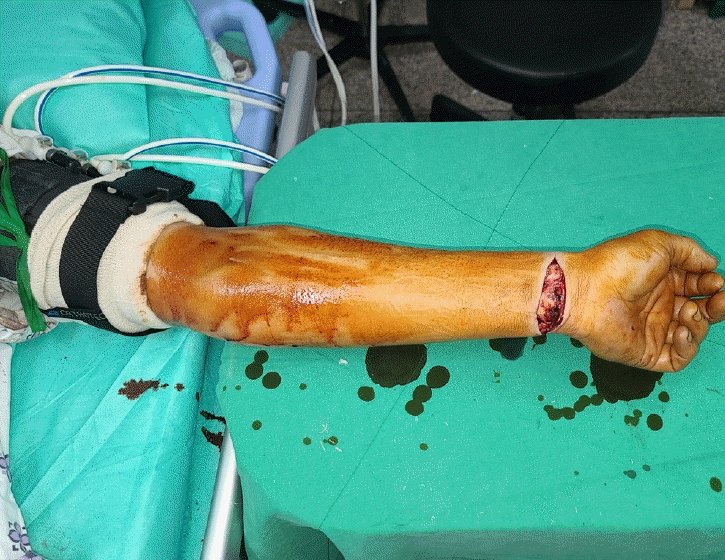
A 57-year-old male Asian patient with major depressive disorder and liver cirrhosis presented to the emergency department after cutting himself on his left wrist with a knife. The patient had been diagnosed with COVID-19 three days prior and was in quarantine. Compression was performed to stop active arterial bleeding but failed to control the hemorrhage. The patient’s blood pressure dropped from 100/60 mmHg at arrival to 70/40 mmHg. Although emergency surgery was necessary to achieve hemostasis, the OR at our hospital was not equipped with negative pressure equipment, so patients with COVID-19 were not allowed to enter. Therefore, we decided to perform emergency surgery in the isolation room of the emergency department under IVRA, using a double pneumatic tourniquet (Fig. 1) and tourniquet machine brought from the OR. The surgeon (IK), who also performed the IVRA, wore a Level D protective suit and an N95 mask. An emergency medicine physician was to help in the event of anesthetic complications. Standard monitoring equipment was applied to the patient (electrocardiography, noninvasive blood pressure, and pulse oximetry). For IVRA, an intravenous (IV) catheter was inserted into the dorsum of the left hand, the side where surgery was required, and secured with tape. The double pneumatic tourniquet was applied to the proximal part of the upper arm (Fig. 2). The upper extremity was exsanguinated using an elastic bandage, and the proximal cuff of the double pneumatic tourniquet was inflated to 250 mmHg. After the distal arterial pulse was checked to confirm that the cuff was properly inflated, 40 mL of 0.5% lidocaine (200 mg) was slowly injected during approximately 90 seconds through the IV catheter. The IV catheter was removed from the left-hand dorsum, and after waiting for approximately 10 minutes, anesthesia was confirmed. The distal cuff of the double pneumatic tourniquet was inflated to 250 mmHg and the proximal cuff was deflated, after which emergency surgery was then initiated. The ulnar artery and vein were both injured with concomitant multiple tendon injuries (palmaris longus, flexor carpi ulnaris, and 3, 4th flexor digitorum superficialis). After ligating the injured blood vessels, the surgeon decided to perform additional surgery for the damaged tendons after quarantine was finished. The total operative time was 18 minutes. To prevent anesthetic complications, the tourniquet was deflated after waiting up to 30 minutes from injection. The patient experienced dizziness for approximately 10 minutes after the tourniquet was released but recovered and had no other complications. Postoperative hospitalization was not possible due to the lack of isolation wards. Therefore, a dorsal block splint was applied, and the patient returned home. His quarantine ended 11 days later, after which tenorrhaphy was performed in an OR under brachial plexus block. Postoperatively, the patient received professional rehabilitation care, and his functional prognosis was favorable.
Case 2
A 37-year-old female Asian patient with major depressive disorder presented to our emergency department after cutting herself on her right wrist with a knife. She had been diagnosed with COVID-19 six days prior to the injury and was in quarantine. Active arterial bleeding was observed on arrival, and her blood pressure dropped to 70/40 mmHg. We decided to perform an emergency operation under IVRA in the isolation room. Another self-inflected laceration on the right-hand dorsum prohibited insertion of an IV catheter there, therefore the catheter was inserted into the right antecubital vein. IVRA was performed in the same manner as in case 1, after which injuries to the ulnar artery and multiple tendons (palmaris longus, flexor carpi radialis and flexor carpi ulnaris) were confirmed by surgical exploration. The injured vessel was then ligated. The total operative time was 16 minutes. Again, the tourniquet was deflated after waiting up to 30 minutes from the injection time to prevent anesthetic complications. The patient recovered uneventfully from IVRA. A dorsal block splint was applied, and the patient was sent home. Eight days later her quarantine period was finished, and tenorrhaphy was performed in the OR. The patient displayed favorable functional recovery after rehabilitation.
Case 3
A 39-year-old female Asian patient without any underlying diseases was admitted to the emergency department. The patient had injured her left wrist while working with a grinder. Emergency surgery was required for active arterial bleeding which was causing her blood pressure to drop. However, her temperature was 38.4 °C. According to hospital regulations, she was not allowed to enter the OR until a polymerase chain reaction test for COVID-19 was verified. Therefore, we decided to perform emergency surgery under IVRA in the isolation room. After inserting an IV catheter into the left-hand dorsum, IVRA was performed in the same way as in case 1. The radial artery, nerve and first extensor tendon compartment were damaged. The injured radial artery was ligated, and tenorrhaphy was performed on the injured tendons. The total operative time was 48 minutes. After tourniquet release, the patient recovered without any complications. The next day, her COVID-19 polymerase chain reaction test result was confirmed negative, and neurorrhaphy was performed in the OR.
Discussion
IVRA is a useful anesthesia method for upper or lower extremity surgery that takes less than an hour (this is because the tourniquet must remain inflated to maintain anesthesia). It is known to be safe for emergency room settings [3-5] and can also be safely used in pediatric surgery by adjusting the dose of local anesthetic (LA) [3].
Several studies have previously described the IVRA method for upper extremities in detail [5-8]. An IV catheter is inserted into the dorsum of the extremity where surgery is required. Subsequently, a double-pneumatic tourniquet is applied to the proximal part of the upper arm. After exsanguination using an elastic or Esmarch bandage, the proximal cuff is inflated to 250 mmHg. Before injecting LA intravenously, it is essential to ensure that the tourniquet is properly inflated because LA spreads into the general circulatory system throughout the body when tourniquet leakage occurs. LA is then injected into the IV line. Typically, 40 mL of 0.5% lidocaine (200 mg) is administered. The maximum recommended dose of lidocaine is 3 mg/kg [8]. The onset of anesthesia occurs within 5 to 10 minutes [8], after which the proximal cuff of the tourniquet should be inflated and the distal cuff deflated. This alternate inflation process is required to maintain anesthesia without tourniquet pain. During surgery, other physicians or trained nurses should monitor the patient. When the operation is complete, the tourniquet is deflated slowly, and the patient should be closely monitored for 30 minutes [7].
The IV catheter is typically inserted into the dorsum of the ipsilateral hand. If this location is not feasible, the catheter may be inserted into the antecubital or other veins. Catheter location does not affect IVRA success rate [9]. However as failing to insert the IV catheter results in anesthesia failure, personnel skilled in catheter insertion should perform the procedure. Another IV catheter must also be inserted into the contralateral upper or lower extremities. This is because emergency IV access may be required due to anesthesia complications.
Exsanguination of the upper extremity is another important preliminary step for IVRA. Exsanguination drains blood from the upper extremities and veins, leading to capillary collapse. Because only a small amount of LA is used during IVRA, the quality of anesthesia can be improved when exsanguination is properly performed [7]. However, exsanguination with an Esmarch or elastic bandage can be painful, particularly in patients with open wounds. A 2008 study demonstrated no difference between exsanguination using an Esmarch bandage and upper extremity elevation at 90° for 5 minutes [10].
Lidocaine is the most commonly used LA in IVRA [4,7,8]. Prilocaine was previously also widely used, but was withdrawn in North America due to methemoglobinemia side effects [8]. Bupivacaine is also contraindicated for IVRA [4,7,8]. If surgeons have to perform IVRA themselves, it is best to use lidocaine, which is considered to be the safest. LA exerts its effects by attaching to the intracellular domains of Na+ channels, blocking neuronal ion transfer, depolarization, and neuronal transmission [11]. LA injected intravenously for IVRA spreads retrogradely into the collapsed capillaries and soft tissue. Through this process, it acts on sensory receptors in the dermis as well as directly on nerve trunks via the epineural vessels.
The tourniquet should be released slowly after surgery since systemic complications can occur when a large amount of LA suddenly spreads throughout the general circulatory system. Tourniquet deflation should be done at least 15 to 30 minutes after LA injection because it takes time for LA to bind sufficiently to tissues [4,5,7,8,12]. To prevent anesthesia complications, the authors released the tourniquet 30 minutes post-injection in all patients, and closely monitored the patient for at least 30 minutes [7,12].
IVRA has several advantages [7,8]. It is safe, with a low incidence of systemic toxicity and a shallow learning curve. The onset time is short. After surgery, the patient recovers quickly from anesthesia. In addition, because anesthesia is initiated after tourniquet inflation, it is particularly advantageous for bleeding control, especially in patients with active arterial bleeding.
Contraindications for IVRA are presented in Table 1 [4,7,8]. Some studies have described open wounds as an absolute contraindication [7,13]. These reports explain that this is because the injected LA may leak out from the wounds. However, most studies do not state open wounds as a contraindication. In the authors’ experience, IVRA was successful in all patients with open wounds. If the patient has an open wound, vein selection for catheterization should be carefully based on the mechanism of IVRA. Veins immediately proximal to the open wound should be excluded to avoid venous leakage of LA.
The success rate of IVRA has been reported to be >96%. The complication rate was less than 2% and most complications were minor ones [6,8]. As such, IVRA is known to be a very safe procedure. However, major complications can occur in rare cases. Before starting IVRA, standard monitoring equipment for electrocardiography, noninvasive blood pressure, and pulse oximetry should be applied to the patient. This is to monitor against potential major anesthetic complications. In addition, surgeons who perform IVRA must obtain an advanced life support certification. The most common complication of IVRA is systemic leakage of LA [7,8,12,14]. When tourniquet leakage occurs during surgery, or when the tourniquet is released after surgery, a large amount of LA may enter into the body’s circulatory system. Systemic LA leakage affects the central nervous system and cardiovascular system [8,11]. As the plasma concentration of LA rises, excitatory pathways are affected, producing a depressive phase of neurological toxicity [11]. Due to this central nervous system toxicity, minor complications such as tinnitus, dizziness, and metallic taste in the mouth, as well as major complications including loss of consciousness, seizure, coma, and respiratory arrest may occur [8,11]. In the cardiovascular system, LA molecules can cause conduction disturbance and myocardial dysfunction through Na+ channel blockage [8]. Prolonged PR, QRS, and ST intervals appear on electrocardiography [11]. In addition, LA blocks calcium channels and Na+-Ca2+ exchange pumps in myocardial cell membranes [11], lowering intracellular calcium concentrations. As a result, myocardial muscles lose contractility, leading to myocardial dysfunction. These mechanisms can cause chest pain, bradycardia, and cardiac arrests [8,11]. If complications occur, surgery should be stopped immediately and help should be sought. The airway should be secured, and 100% oxygen administered to reduce the blood flow and hence LA uptake into the brain [15]. IV lipid emulsion therapy can also be considered if cardiac effects persist [11,14]. In case of cardiac arrest, an Advanced Cardiac Life Support algorithm for cardiopulmonary resuscitation should be followed [11]. If a seizure occurs, it is important to terminate it quickly, and benzodiazepines are the first-line therapy [11,12]. Therefore, it is important to seek help from emergency medicine physicians or anesthesiologists for professional treatment.
In case 1, dizziness occurred after tourniquet release. The patient had liver cirrhosis which would have weakened the metabolic function of the liver. Pharmacokinetically, lidocaine is metabolized in the liver and is excreted by the kidneys [11]. Although the tourniquet was released after a sufficient period of time, the authors presume that systemic toxicity occurred due to the slow metabolism of lidocaine caused by weakened liver function. Therefore, the amount of LA injected should be reduced in patients with liver dysfunction.
Due to the COVID-19 pandemic, hospitals lacking negative pressure equipment in their OR cannot offer emergency surgery on patients with COVID-19 infection. Basically, for safety, anesthesia must be performed by an anesthesiologist in the OR. However, if a patient who requires emergency surgery cannot enter the OR, IVRA is a relatively safe method that the surgeon can perform directly without an anesthesiologist.