Early Compression Therapy for Deep Skin Defects: A New Treatment Option to Prevent Hypertrophic Scars or Contractures
Article information
Abstract
Background
Conservative treatment of deep dermal or full-thickness skin defects often results in hypertrophic scars or contractures; thus, compressive therapy has been used after wound closure to prevent or treat scar deformities. However, wound contraction begins in the early proliferative phase and peaks after 2 weeks. We therefore attempted early compression therapy as a means of conservative treatment of deep-skin defects and evaluated its clinical outcomes.
Methods
In 21 cases of deep skin defects (19 patients), early compressive therapy was started the second week after injury. Saline-moistened gauze or foam dressings were placed on open wounds, and foam dressings or silastic plates were used after epithelialization. The compression materials included elastic bandages, adhesive tapes, or garments. The final scars were assessed using the Vancouver Scar Scale (VSS) and satisfaction degree.
Results
Defect size ranged from 1.4×0.7 to 5×5 cm. The duration of compression was 4 to 12 months. The follow-up periods were 4 to 61 months. Mild scar hypertrophy or contracture occurred in 15 cases and subsided after application of topical corticosteroid or triamcinolone injection. The final scar shapes were linear (n=12), geographic (n=5), and oval (n=4). The mean VSS score was 2.3. The degrees of satisfaction were excellent (61.9%) and good (23.8%). In most cases, aesthetically and functionally satisfactory outcomes without pathologic scars were demonstrated with minimal scar size, high scar quality, and high satisfaction.
Conclusion
Early compression therapy might be a good option to prevent pathologic scars in the conservative treatment of deep skin defects.
Introduction
In the treatment of deep skin defects, including full-thickness defects, secondary intention by conservative management is an alternative option for patients unsuitable for surgery due to refusal or poor condition.
Deep skin defects usually heal through granulation tissue formation, wound contraction, and epithelialization [1–7]. Wound contraction is an important part of the healing process for deep or full-thickness skin defects, in which the surrounding skin is pulled circumferentially toward an open wound [3,4]. It can dramatically decrease wound size without granulation tissue formation and close the wound more rapidly than epithelialization alone [4,5]. However, human skin is firmly attached to the underlying tissue layer. Therefore, wound contraction is limited by counter-tension due to poor skin mobility [2,4], which consequently accelerates myofibroblast activity and granulation tissue formation and induces intense contraction forces and scar formation [6–8], resulting in a high risk of scar hypertrophy or contracture. Furthermore, if wounds remain open for over 2 weeks, the incidence of hypertrophic scars will dramatically increase due to prolonged inflammation [9].
Compression therapy has traditionally been used as an important nonsurgical therapeutic regimen to prevent or treat scar contracture or hypertrophy. Many studies have reported that compression can accelerate the remodeling and scar mat-uration processes with collagen rearrangement, resulting in scar improvement [10–16]. However, traditional compression therapy is used in the late stages of wound healing after complete epithelialization or wound closure occurs.
Myofibroblasts play a key role in the wound contraction and pathologic contracture observed in hypertrophic scars [3,4,6,7]. They appear in acute wounds 4 to 5 days after wounding, and their quantity peaks 2 weeks after wounding occurs [3,4]. This may indicate that wound contraction begins at an early stage of the wound healing process and peaks at 2 weeks after wounding [3]. Thus, we believe that compression therapy should be started from an early stage of the wound healing process to enable the more effective prevention of contracture or hypertrophic scar, especially on the face, hands, and feet.
This study aimed to introduce compression therapy associated with conservative wound treatment at an early stage in deep dermal or full-thickness skin defects and evaluate its clinical outcomes.
Methods
The current study included 21 cases of deep dermal or full-thickness skin defects in 19 patients (11 male, 8 female) aged 8 days to 53 years. The defects were caused by deep abrasion (n=8), extravasation (n=6), deep burn (n=4), avulsion (n=2), and dog bite (n=1) (Table 1). The study was approved by the Institutional Review Board of Kyung Hee University Medical Center (IRB file No: 2022-01-001). The patients provided writ-ten informed consent for the publication and the use of their images.
All defects were treated with conservative management and healed by secondary intention because of patient/parent refusal or ambiguous wound conditions. During the first week, after cleansing with normal saline, sufficient amounts of anti-in-flammatory (beta-sitosterol) and antibiotic (mupirocin) ointments were applied to the wounds and adjacent skin regions, followed by coverage with saline-moistened gauze dressings. This treatment was performed once or twice a day to absorb exudates and prevent inflammation. Upon being clearly de-marcated, the necrotic tissues were removed. Patients with extravasation and other large wounds were generally treated as inpatients, while those with small wounds were treated as out-patients.
Compression therapy was initiated the second week after wounding. After the application of two topical ointments to wounds and adjacent skin regions, thick non-adhesive poly-urethane foam or saline-moistened gauze dressings were applied as inserts to provide definitive pressure and ensure smooth and non-abrasive contact surfaces between wounds and compression materials. Various types of elastic bandages, adhesive skin tapes, and compression garments were used as compression materials. When compression materials were applied, care was taken to avoid the application of excessive pressure, considering the additional pressure induced by their thickness. The degree of pressure was determined and readjusted according to the wound condition to prevent ischemia, provide a flat surface, and slow the wound contraction with loosening of the surrounding skin. The endpoint of compression was a little tightness on the inserts and minimal tightness on the normal skin beyond them. Frequent follow-up was performed every few days or weeks to monitor the healing process and pressure adequacy.
Once the wounds had epithelialized, the patients were in-structed to thoroughly cleanse the scar area with tap water and soap and apply topical beta-sitosterol ointment or moisturizing cream to soften the scar and adjacent skin regions while protecting the fragile scar epithelium. The compression therapy was continued in the same manner for the extremities. In concave or convex areas of the face, such as the philtrum, lip, or malar area, silicone thermoplastic splints (Silon-STS; Bio Med Sciences, Allentown, PA, USA) were used as inserts and adhesive paper tapes were used as pressure materials [17]. The materials were molded after heating depending on the surface shape of the scar area to provide definitive and even pressure to the scars and surrounding skin. The patients were instruct-ed to open the scar area for 4 hours/day to prevent irritation or eczema due to overhydration. Otherwise, the recommended compression time was 20 hours/day.
During the follow-up period, the scars were frequently monitored for any signs of irritation, maceration, or hypertrophy. When signs of irritation appeared, topical hydrocortisone cream was administered. When mild scar hypertrophy or contracture (tissue distortion or contraction band) occurred, strong corticosteroid cream (clobetasol propionate) was topi-cally applied for 2 weeks with readjustment of compression materials. When it did not subside, intralesional triamcinolone injection was administered every month until the scar was flat, soft, and stable. The inserts were readjusted to accom-modate receding scars and maintain definitive contact with the scar surface. The fit of the pressure garments was also checked to determine whether readjustment or replacement was required. The compression therapy was continued until the scar was soft, flat, and light pink or white.
Defect location, size, and depth, epithelialization time, compression duration, presence of hypertrophic scar or contracture, and final scar shape were reviewed in the patients’ medi-cal records and photographs. For objective evaluation of clinical outcomes, the final scars were assessed and graded using the Vancouver Scar Scale (VSS) at the last follow-up. VSS included pigmentation (0, normal; 1, hypopigmentation; 2, hy-perpigmentation), pliability (0, normal; 1, supple; 2, yielding; 3, firm; 4, banding; 5, contracture), height (0, flat; 1, <2 mm; 2, 2–5 mm; 3, >5 mm), and vascularity (0, normal; 1, pink; 2, red; 3, purple) [18]. The scores for each parameter were assessed separately. All four scores were summed. For the sub-jective evaluation, the patients or parents were surveyed for their satisfaction at the last follow-up. Satisfaction was graded as excellent, good, fair, or poor.
Results
There were 21 cases of deep dermal (n=7) or full-thickness (n=14) skin defects in 19 patients, including those on the foot or ankle (n=10), hand (n=7), and face (n=4) (Table 1). Defect size ranged from 1.4×0.7 cm (finger dorsum in a baby) to 5×5 cm (foot dorsum in a baby). Epithelialization was complete at 18 to 55 days. Compression therapy duration was 4 to 12 months, while follow-up duration was 4 to 61 months.
The final scar was linear in 12 cases (57.1%), geographic in five (23.8%), and oval in four (19.1%). Most cases of linear scars resulted from a full-thickness defect that was closed by gradual migration of the flexible surrounding skin due to wound contraction with minimal granulation tissue formation and marginal epithelialization (Figs. 1, 2). Geographic scars resulted from deep dermal defects, full-thickness defects with limited skin laxity, or large full-thickness defects with flexible skin laxity (Fig. 3). Oval scars resulted from oval-shaped deep dermal or full-thickness defects with limited skin laxity (Fig. 4). Final scar size was 10% or less of the initial defect size in 14 cases, 20% in one, 50% to 60% in four cases and 80% in two cases (Table 1).
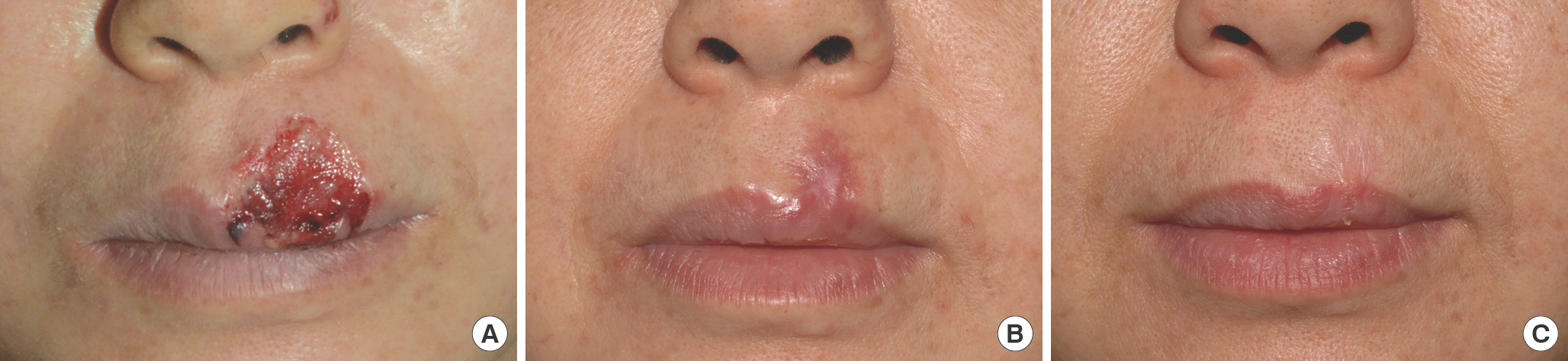
Case 1 of a linear scar (patient 19). (A) A 53-year-old female with a full-thickness skin defect (2×2 cm) on the upper lip caused by a dog bite. (B) Epithelialization was complete at 3 weeks after injury. Compression therapy was continued using a silicone splint and paper tapes for 8 months, associated with triamcinolone injection four times. (C) One year later, a stable linear scar remained without contracture. Vancouver Scar Scale score was 2 and patient satisfaction was excellent.
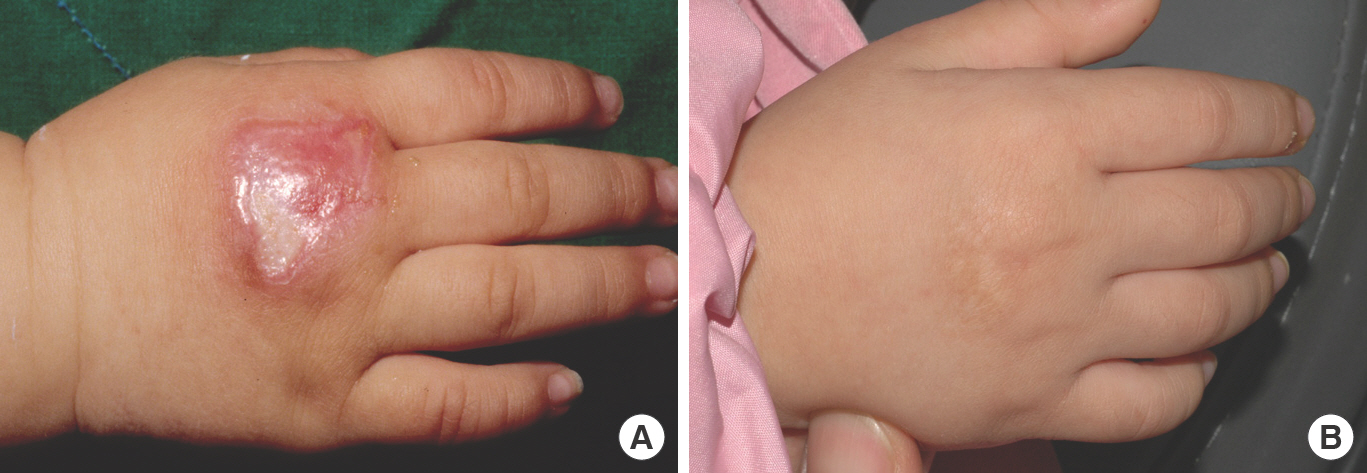
Case 2 of a linear scar (patient 3). (A) A 14-month-old female with deep abrasion (2×1.5 cm) on the hand dorsum from a treadmill belt injury. Complete epithelialization was achieved 23 days after injury. Compression therapy was administered for 6 months. (B) Thirty-four months later, a linear hypopigmented scar remained. Vancouver Scar Scale score was 1 and parent satisfaction was excellent.
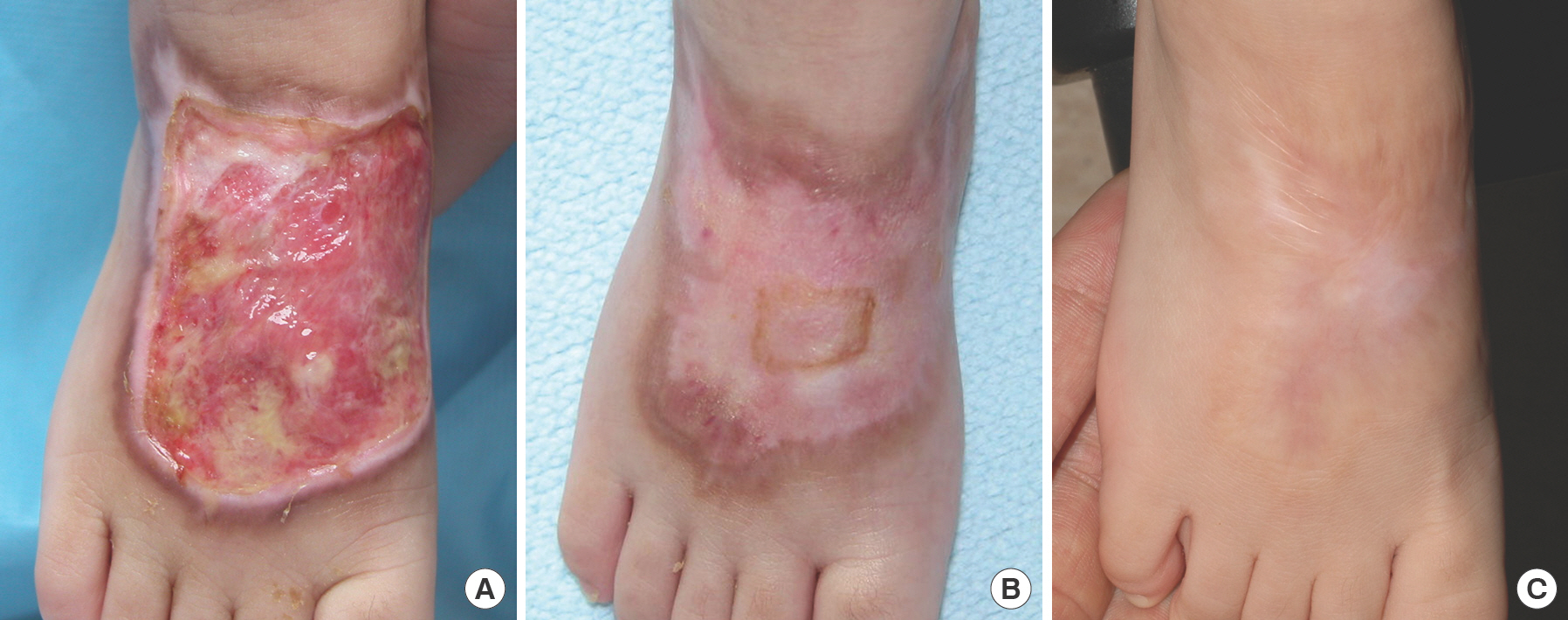
A case of a geographic scar (patient 11). (A) A 1-year-old male with full-thickness skin necrosis (5×4 cm) on the foot dorsum caused by potassium chloride extravasation. After removal of the eschar, early compression therapy was started using foam or saline gauze dressing and elastic bandages. (B) Epithelialization was complete 55 days after the injury. Compression therapy was continued for 1 year using a polyurethane foam dressing and a pressure garment with one triamcinolone injection. (C) Thirty-two months after the injury, a stable geographic scar remained with marginal skin wrinkles. Vancouver Scar Scale score was 4 and parent satisfaction was fair.
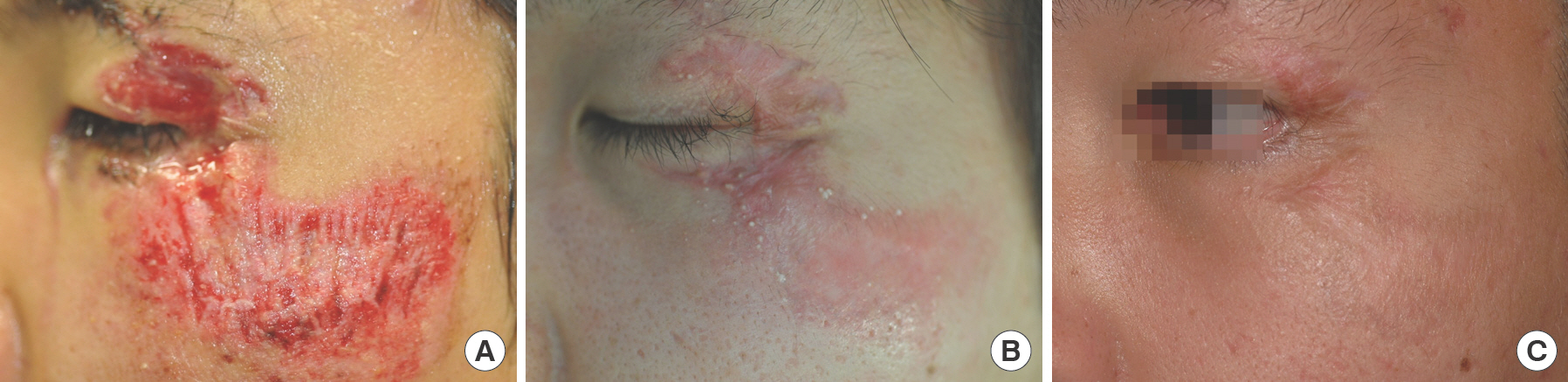
A case of an oval scar (patient 2). (A) An 18-year-old male with a deep dermal defect (4×2 cm) on the zygoma and a full-thickness skin defect on the eyelid caused by a deep abrasion. Epithelialization was complete 18 days after injury. (B) Mild hypertrophic scars and moderate eyelid contraction appeared, for which three triamcinolone injections were performed. Compression therapy with silicone thermoplastic splints was continued for 8 months. (C) One year later, an oval scar on the malar area remained, while a stable geographic scar on the eyelid remained with mild eyelid distortion. Vancouver Scar Scale score was 2 on the zygoma and 6 on the eyelid. Patient satisfaction was excellent and good respectively.
Mild scar hypertrophy or contracture appeared as the initial stage in 15 cases during compressive therapy managed by patients themselves or their parents. It subsided in six cases but not in nine cases at 2 weeks after topical application of strong corticosteroid cream and readjustment of compression materials. In nine cases, it subsided after triamcinolone intralesional injection, once in four cases and two to four times in five cases (Table 1). Minimal contracture with mild structural distortion occurred in one case of full-thickness skin defect of the eyelid (Fig. 4). However, there was no functional deformity even among the large defects.
The final scar VSS score was 1 in seven cases, 2 in eight cases, 3 in two cases, 4 in two cases, 5 in one case, and 6 in one case, resulting in high-quality final scars (mean=2.3). Patient or parent satisfaction was excellent in 13 cases (61.9%), good in five (23.8%), fair in three (14.3%), and poor in none. The satisfaction degree in the six cases of extravasation (3 good and 3 fair) was significantly lower than in 15 cases of injury by themselves (13 excellent and 2 good). However, all patients were satisfied with the final aesthetic and functional results compared to the severity of the initial defects.
Discussion
Deep skin defects, including full-thickness defects, are caused by various injuries, such as mechanical, thermal, chemical, and ischemic injuries. Various surgical techniques, such as primary closure, skin grafting, or flap surgery, are generally used to treat deep skin defects while minimizing sequelae, such as hypertrophic scars, skin distortion, or contracture. However, when patients are unsuitable candidates for surgery, secondary intension healing by conservative management is the only treatment option, for which it is challenging to prevent aesthetic or functional sequelae.
The wound healing process involves the inflammatory, proliferative, and remodeling phases [1–4]. During the proliferative phase, wounds are closed by epithelialization, granulation tissue formation, and contraction [1–7]. The contribution of each process of the proliferative phase to wound healing varies among wound types. Epithelialization is the main contributor to wound healing in partial-thickness skin defects, where skin appendages remain. However, in deep or full-thickness skin defects, wound contraction, in which the surrounding skin is pulled circumferentially toward an open wound, is an important part of the healing process. It dramatically decreases the wound size without granulation tissue formation. It also makes the scar size smaller in the early stage of the remodeling phase [4,5].
Wound contraction is also related to skin mobility [2,4]. Other animals have a much greater capacity for wound contraction than humans do [4]. Most mammalian animals have a panniculus carnosus, a myofascial layer between the subcutaneous fat and musculoskeletal layers [4]. This low-resistance plane can enhance skin mobility and wound contraction [4]. Premature infants also have a greater capacity for wound contraction than adults [5]. Their skin has less tensile strength with a greater degree of laxity and mobility because it is thin and wrinkled with a small amount of subcutaneous fat due to its immaturity [5]. Thus, defect closure in premature infants is mainly dependent on wound contraction, even in extensive full-thickness defects, resulting in less scarring and a lower incidence of loss of function [5]. This suggests that laxity or mobility of the surrounding skin is very important for decreasing scar problems in deep skin defects.
In human adults, wound contraction is greatest in the trunk and perineum, intermediate in the head and neck, and limited in the extremities due to differences in skin mobility [2,4]. It can contribute to up to 80%–90% of the decrease in wound size in the trunk and perineum. In the face and extremities, where the skin is firmly attached to the underlying tissue layer, wound contraction is limited by counter-tension due to poor skin mobility. This causes the tissue to be under high levels of mechanical stress. Myofibroblasts are over-activated, consequently inducing cell proliferation, intense contraction forces and scar collagen formation [6–8]. Furthermore, delayed epithelialization beyond 2 weeks increases the incidence of hypertrophic scar owing to prolonged inflammation [9].
In this study, to minimize or prevent pathologic scar, we attempted conservative wound management with three con-cepts: anti-inflammation, moisturizing the surrounding skin, and early compressive therapy, at least until the scar was stabi-lized.
Although inflammation is an important event in adult wound healing, a lack of inflammation plays a key role in scar-less wound healing in the early fetus [2,5,19,20]. As the amount of inflammation is closely related to scar formation, intense inflammation can induce excessive granulation tissue formation and consequent fibrosis or hypertrophic scar formation [19,20]. All deep defects in this study were expected to be closed beyond 2 weeks; consequently, intensive granulation tissue and scar formation due to prolonged inflammation were observed. Thus, we performed intensive inflammatory treatment in the inflammatory and proliferative phases. Intensive moisturizing of the surrounding skin may increase its laxity and mobility; consequently, this may permit wound healing by wound contraction without skin distortion or scar contracture, similar to the skin wound healing that occurs in animals. For this reason, topical anti-inflammatory agents were applied to the surrounding skin and covered with dressing materials in the same manner as for wound management.
In our experience, hypertrophic scar formation or scar contracture is not often prevented by only anti-inflammatory treatment and skin moisturizing. Therefore, early compression therapy as a powerful additional means of treatment is required to decrease the counter-tension by the surrounding skin, to lessen the intensity of contraction forces relative to skin laxity, and quickly realign coarse scar collagen bundles in a flat reticular pattern. To ensure successful compressive therapy, the fit of compression materials and degree of compression force should be considered [13]. Compression therapy is achieved by the outer compression materials as well as their inner inserts. The inserts, which are applied to the wound or scar and the surrounding skin, are in direct contact with these targets and actually compress them using the compression force of the outer compression materials. Soft silicone sheets were not used as inserts because of skin problems caused by intensive hydration and ineffective compression. When compression materials are applied, excessive pressure should be avoided to prevent ischemia or ulcers being induced by additional pressure from the extra thickness of the inserts. In this study, an elastic mesh or net-type bandage with relatively low tightness was used. Compression garments or stockings were used in a larger size (one or two levels) than the originally recommended size of their series. Though the compression degree was moderately tight on the inserts and slightly tight on the normal skin outside them, it was readjusted depending on the wound or scar status during follow-up. Compression pressure was not measured because of practical difficulty and its questionable significance.
Topical application of potent corticosteroid creams and intralesional injection of triamcinolone seems to have an important role in inhibiting hypertrophic scar or contracture ap-pearing in the early stage of remodeling phase after epithelialization. Corticosteroid suppresses inflammation, is a vasocon-strictor and has an anti-mitotic effect that inhibits new collagen formation and decreases scar mass. In this study, potent corticosteroids were applied immediately in 15 cases where the initial stage of hypertrophic scar or contracture occurred during compressive therapy managed by patients or their parents, and in terms of final outcomes, resulted in minimal contracture without functional deformity in only one case of larger full-thickness eyelid defect.
Early compression therapy from the early second week after wounding was provided with local wound treatment in 21 cases of deep dermal or full-thickness skin defects on the face, hand, and foot for more effective prevention of hypertrophic scar and contracture and continued for 4 to 12 months. In most cases, aesthetically and functionally satisfactory outcomes with just one case of minimal contracture without functional deformity were demonstrated with minimal size and high quality of the final scar, as well as a high degree of patient/parent satisfaction compared to the severity of the initial defect. Our findings suggest that early compression therapy might be a good option to prevent hypertrophic scar or contractures as nonsurgical conservative treatment of deep dermal or full-thickness skin defects.
Our study has some limitations. The sites, causes and sizes of the defects were variable, and the small number of cases and wide distribution of age may also make the result statistically significant or inaccurate because of insufficient data. Another limitation is the lack of a control group in which compression therapy is applied after occurrence of hypertrophic scar or contracture during long-term conservative wound management without intensive therapy or surgery. We expect a pio-neer to establish a control group with a large number of cases in the future.
Notes
No potential conflict of interest relevant to this article was reported.

