 |
 |

|
| Aims and Scope |
| About the Journal |
| About the Society (KWMS) |
| Editorial Board |
| Open Access |
| Principles of Transparency and Best Practice |
| Editorial Office |
| Subscriptions |


|
| Aims and Scope |
| About the Journal |
| About the Society (KWMS) |
| Editorial Board |
| Open Access |
| Principles of Transparency and Best Practice |
| Editorial Office |
| Subscriptions |

AbstractBackground Drains are hypothesized to cause surgical site infections (SSIs). However, research is scarce on how to reduce SSIs after drain placement. We analyzed the association between specific drain characteristics and the occurrence of SSI. We also evaluated the effects of other known risk factors in patients undergoing plastic surgery to reduce SSIs.
Methods We retrospectively reviewed the medical charts of 531 patients who underwent plastic surgery with drain placement between January 2017 and January 2022. Data were analyzed using the chi-square test or Fisher exact test for categorical variables and the Mann-Whitney U test or t-test for numerical variables.
Results SSI incidence was higher in closed drains (15.4%) than in open drains (8.0%). SSIs also occurred more often after delayed drain removal. For open drains, early removal did not decrease SSI incidence. For closed drains, SSI incidence was markedly high when the drain was removed after 6 days. Furthermore, bacterial culture results tended to differ before and after SSI occurrence more frequently in the open drain group. Among the known risk factors for SSIs, smoking, albumin concentration, and wound status were confirmed as significant.
Conclusion Drain removal time was a significant risk factor for SSIs. With open drains, it is important to assess whether SSI occurs at the beginning of drain placement. A higher probability of retrograde infection was confirmed with open drains. Closed drains should be removed within 6 days after placement. Furthermore, smoking, albumin concentration, and wound status should be considered to reduce the incidence of SSIs.
IntroductionSurgical site infections (SSIs), defined as infections that occur within 30 days of undergoing surgery or within a year of inserting an implant in the surgical field, are common healthcare-associated infections, affecting nearly 3% to 20% of surgical cases [1,2]. SSIs are associated with increased morbidity and mortality, ranging from superficial skin infections with wound discharge to life-threatening conditions such as severe sepsis [3]. Significant advances have been achieved in recent years toward reducing SSIs, with several studies published on SSI risk factors [4]. Despite these advances, the incidence of SSIs remains high owing to other factors, such as more aggressive interventions performed in patients with increasingly worse clinical conditions.
Drains are commonly used in surgical procedures to prevent abscesses or hematomas. However, drains are hypothesized to cause SSIs through external or luminal contamination, followed by retrograde bacterial migration along the drain surface [5]. Among the studies that examined SSI risk factors, some have also assessed the correlation between drain placement and SSI occurrence. Despite repeated failures in previous studies to demonstrate a clear benefit, drains are still commonly used in surgery [6]. This is even more so in plastic surgery which frequently involves extensive tissue dissection and the creation of equally large potential spaces. However, there is a lack of studies presenting objective analysis of drain placement in plastic surgery. Additionally, only a few studies have examined the effect of drain-specific factors (such as type, number of drains, and removal time) on the occurrence of SSI in other surgical disciplines such as orthopedic, vascular, and general surgery. A small number of studies have reported an increased risk of SSIs associated with open drains [7]. To date, studies have primarily focused on examining the effects of drain placement on the occurrence of SSIs, and the results have yielded inconsistent results. Furthermore, research clarifying points to be considered to reduce the occurrence of drain-associated SSIs is inadequate. This could be one of the reasons why drain placement is mainly left to the surgeon’s discretion.
Knowing the drain-specific factors that affect the occurrence of infections can help reduce SSIs by allowing surgeons to monitor them after drain placement. The present study analyzed the association between specific drain characteristics and SSI in patients undergoing plastic surgery with drain placement. This study also analyzed the effect of other previously reported risk factors for SSIs in plastic surgery patients to investigate strategies to reduce SSIs.
MethodsPatientsWe retrospectively reviewed the charts of 531 hospitalized patients who underwent surgery in various anatomical regions (such as the head and neck, chest, abdomen, back, buttock, sacral, and lower extremities) with drain insertion at our hospital’s plastic surgery division between January 2017 and January 2022. Exclusion criteria were: (1) patients in whom drain tip culture was not performed after drain removal; (2) patients who could not be followed up until drain removal; and (3) patients whose medical records were deficient in any aspects included in the study. All investigations were performed in accordance with the principles of the World Medical Association Declaration of Helsinki (June 1964) and subsequent amendments. This study was approved by the Institutional Review Board of Wonkwang University Hospital (IRB No. WKUH 2022-08-037-005). Written informed patient consent for the use and publication of clinical images was obtained.
Study designVarious surgeries were performed in the included patients, including excision and biopsy (for lesions such as skin cancers, epidermoid cysts, and lipomas), debridement (for abscess pockets, diabetic foot ulcers, pressure injury site, etc.) and flap surgery (such as local advancement flaps, rotational flaps or distant flaps), breast implant insertion, and amputation. Two types of drains were used: open drains (a silicon drain adjusted to the wound size) (Fig. 1A) and closed drains (Hemovac; MOOHAN M-VAC, Model No.: PP200L, PP400L) (Fig. 1B). Open drains were removed after confirming no specific drain discharge or if the drain irritated the wound. In closed drains, the drains were removed when the output decreased below 20 mL/day for two consecutive days. Drain tips were aseptically cultured upon removal to analyze causative pathogens of the SSIs. A plastic surgery resident and professor observed the patients’ surgical wounds daily from the day after surgery until discharge to detect any SSIs. Wound status and wound dressing technique were recorded. We also examined wound conditions in the outpatient clinic after the patients were discharged and recorded any SSI incidence. SSIs were defined (Fig. 2) by culture-positive findings with purulent drainage from the surgical site or with at least one of the clinical signs of infection, such as pain or tenderness, localized swelling, redness, or heat according to the definition of SSI by the Centers for Disease Control and Prevention (CDC) [8].
Based on the above methods, the association between specific drain factors (type, number, and time of removal) and the occurrence of SSI after drain placement were analyzed. We also performed a chart review of patient characteristics (age, sex, body mass index [BMI], use of alcohol/tobacco, and serum albumin level) [9-11] and underlying diseases (hypertension [HTN], diabetes mellitus [DM], chronic obstructive pulmonary disease [COPD], ischemic heart disease [IHD], congestive heart failure [CHD] and chronic kidney disease [CKD]) [9], which are known to increase the risk of SSIs. Operation-related risk factors for SSI were also analyzed, such as duration of surgery and wound class according to the CDC wound classification system (clean [I], clean-contaminated [II], contaminated [III], and dirty [IV]) [9]. As mentioned above, pathogens isolated by drain tip culture were also investigated to analyze the differences in causative bacteria of SSI between the open and closed drain groups. Furthermore, the pathogens isolated from bacterial swab cultures performed before (of wounds clinically infected at initial presentation) and after SSI (from drain tip or discharge cultures of wounds with confirmed SSI) were analyzed to determine the possibility of retrograde infection caused by drains in both groups.
Statistical analysisThe association between the occurrence of SSIs and the studied variables was analyzed using the chi-square test or Fisher exact test for categorical variables and the Mann-Whitney U test or independent two sample t-test for numerical variables. Statistical significance was set at P<0.05. Statistical analyses were performed using IBM SPSS version 27.0 (IBM Corp.).
Results
Table 1 illustrates the distribution of patients with drain placement according to surgical site and procedures included in our study. SSI incidence was significantly high in patients who received surgery in the lower extremities (21.1%) or perineum, buttock and sacral area (21.1%) (P<0.001). In terms of surgical procedures, SSI incidence was significantly higher in patients who underwent amputation (21.0%) or debridement and flap surgery (16.6%) (P<0.001). Table 2 summarizes the number of SSI cases (63 patients; 11.9%) in our study. Table 3 briefly outlines the association between SSIs and specific drain factors (drain type, number, and removal time). Considering drain type, there was a significant difference in SSI incidence between the open (8.0%) and closed (15.4%) (P=0.009) drain groups. The incidence of SSI was 10.8% in the single drain group and 17.9% in the group with two drains. However, these differences were not statistically significant (P=0.072). Regarding time to drain removal, the mean days to removal were significantly longer in SSI-confirmed patients (6.24±3.61) and shorter in patients without SSI (4.75±3.78) (P=0.003). Table 4 summarizes the distribution of other known risk factors for SSIs in our patients. There were no significant age differences between the two groups (60.79±18.84 years for SSI-positive patients vs. 61.14±19.43 years for patients without SSI; P= 0.894). The incidence of SSI was significantly higher (15.9%) in male patients than in female patients (7.1%) (P=0.002). There were no significant differences in BMI (22.79±3.98 kg/m2 in SSI-positive patients vs. 23.81±4.23 kg/m2 in uninfected patients; P=0.07). Serum albumin concentration showed significantly lower values in patients confirmed with SSI (3.44± 0.63 g/dL) than in patients with no SSI (3.90±0.55 g/dL) (P< 0.001). The duration of surgery was longer in the SSI group (93.73±58.28 minutes) than in the non-SSI group (81.70± 58.92 minutes); however, the difference was not statistically significant (P=0.064). Smoking was a significant risk factor associated with SSIs occurrence (smoking group 25.3% vs. non-smoking group 9.2%; P<0.001). The incidence of SSIs was lower in patients who used alcohol (9.1%) than in the non-alcohol-use group (12.3%); however, the difference was not statistically significant (P=0.416). We also found that SSI incidence increased significantly with higher wound class (I, 14 [8.0%]; II, 9 [7.1%]; III, 12 [16.4%]; and IV, 28 [17.9]; P=0.007). Table 5 summarizes the distribution of patients with comorbidities associated with SSI occurrence. SSI incidence was higher in patients with comorbidities (HTN present 13.3% vs. absent 10.7%; DM present 14.8% vs. absent 10.6%; CKD present 20.7% vs. absent 11.4%), except for COPD (COPD present 0% vs. absent 11.9%). However, these differences were not statistically significant. The results displayed in Tables 6 and 7 were analyzed to determine whether drain type affected the occurrence of SSIs based on the results in Tables 3 and 4. Table 6 illustrates that closed drains were removed significantly later (7.26±3.58 days) compared to open drains (2.31±1.79 days) (P<0.001) in our study. Table 7 demonstrates that closed drains were used more commonly in worse wound conditions (open drains 12.7% vs. closed drains 14.6% in type III; open drains 25.1% vs. closed drains 33.2% in type IV; P<0.001). Table 8 illustrates the distribution of patients with SSIs according to drain removal time and drain type. In the open drain group, a high proportion of SSI patients had their drains removed earlier (removal on day 1, 20%; day 2, 30%). In contrast, in the closed drain group there was almost no distribution of SSI patients whose drains were removed early (removal on day 1, 0%; day 2, 0%; and day 3, 2.3%), and the distribution was markedly increased in patients whose drains were removed after 6 days (16.3%). Table 9 summarizes the results of drain tip culture after drain removal to investigate the causative bacteria of SSIs in the open- and closed-drain groups. The frequency of isolated bacteria differed between the two groups. In descending order, the pathogens isolated most frequently from the open drains were methicillin-sensitive Staphylococcus aureus (MSSA), Escherichia coli, and Enterobacter faecalis. The bacteria most frequently isolated from the closed drains, in descending order, were MSSA, Pseudomonas aeruginosa, and E. faecalis. Table 10 highlights the differences in bacterial swab culture results before and after the occurrence of SSIs to evaluate the possibility of retrograde (inward) infection through drains. The rate of different culture results obtained before and after the occurrence of SSI was higher in the open drain group (55%) than in the closed drain group (41.9%).
DiscussionAlthough infection control techniques and surgical practices have improved, SSIs remain a significant cause of morbidity and mortality. They also impose a substantial demand on healthcare resources [2]. As mentioned earlier, many studies have examined risk factors underlying SSIs to reduce their occurrence. These studies found that the SSI risk is multifactorial. SSI risk factors can be classified into patient- and surgery-related factors. Concerning patient-related factors, patient characteristics such as age and sex have been identified as risk factors for SSIs in multiple studies [9,10]. Smoking and alcohol abuse in lifestyles have both been reported to be SSI risk factors [9]. Other risk factors such as BMI [9] were also mentioned in the literature and identified as being associated with SSIs. Low serum albumin concentration (malnutrition) is reportedly an important patient-related risk factor [11]. Various comorbidities were consistently associated with SSI incidence. DM was the most frequently considered comorbidity risk factor [9]. Other comorbidities also found to be associated with SSI after adjustment included HTN, IHD, CHD, COPD, and CKD [9]. Patients with multiple comorbidities had further increased risk of SSIs [3]. For surgery-related factors, the SSI rate increased together with CDC classification wound class in early epidemiological studies [12]. Furthermore, increased duration of surgery was also related to an increased SSI risk [2].
In our study, SSI occurrence was slightly higher (11%) than previous studies. This increased SSI occurrence could be due to the inclusion of many patients with higher (worse) wound classes compared to other studies. In a 2019 study by Mujagic et al. [13] that examined the association between drain-specific factors and SSI in other surgical fields, SSI occurrence increased as the number of drains and time to drain removal increased, and also with the use of open drains. Consistent with this study, although a longer time to drain removal was shown as a significant SSI risk factor in our study, there was no statistically significant association between the number of drains and SSI incidence. Another difference with previous studies was that SSI occurrence was higher with closed drains in our study. However, the analyses of drain type and SSI occurrence seen in Tables 6 and 7 confirm that closed drains were commonly removed later than open drains and were used in worse wound conditions. In light of these results, in our study late removal time and wound class were significant risk factors for SSIs in the closed drain group, rather than the closed drain type itself. Therefore, our study confirmed that among the specific drain characteristics, time to drain removal time was a significant risk factor for SSI occurrence.
As shown in Tables 4 and 5, among the other risk factors of SSI confirmed in previous studies, the mean age of SSI patients in our study was 60.79 years, which is very close to the mean age reported in a study Wilson et al. [14]. However unlike previous studies, in which the female sex was a significant risk factor for SSI [15], male sex was found to be a significant risk factor in our study. Our study also confirmed that low serum albumin levels were associated with an increased SSI occurrence rate, similar to previous results [11]. Accordingly, it is important to consider serum albumin levels and correct the nutritional status before and after surgery to help reduce the occurrence of SSIs. Regarding the duration of surgery as a SSI risk factor, although SSI incidence was higher in the group with a longer duration of surgery, the differences were not statistically significant. However, statistically significant results could be obtained if the number of cases increases. In addition, similar to the results of Alexander et al. [16] consistently demonstrating that smoking increases the SSI risk by at least two times, we found that smoking was a significant risk factor for SSIs. This finding further establishes the importance of smoking cessation. Based on our findings, we second the recommendation for cessation of smoking at least 30 days before surgery by Alexander et al. [16].
Consistent with previous studies that linked SSI occurrence with wound class, our study confirmed that worsening wound class was a significant risk factor for SSIs. In light of our results demonstrating that longer times to drain removal and higher (worse) wound class were associated with a higher possibility of SSI, we recommended removing drains as soon as possible in patients with a poor wound class. Furthermore, although there were no statistically significant differences in the occurrence of SSIs between those with and without comorbidities, all patient groups with comorbidities except for COPD showed a higher rate of SSIs than those without comorbidities. However, statistically significant results could also be obtained if the number of cases is increased. In addition, though DM is known as a significant SSI risk factor among comorbidities as mentioned above, the fact that there was no significant difference in SSI occurrence between the groups with and without DM in our study may have been influenced by our efforts to maintain stable preoperative and postoperative blood glucose levels between 100 and 200 mg/dL. These results were also consistent with findings from Alexander et al. [16] which emphasized the importance of glucose control for reducing SSIs by maintaining serum glucose levels to less than 200 mg/dL and hemoglobin A1c to less than 7.0%. Overall, our results confirmed the importance of glucose control in reducing SSIs.
Investigating the relationship between specific drain characteristics and SSI occurrence, which was the primary purpose of our study, objective results were obtained from bacterial cultures, a finding lacking in other studies. The microorganisms cultured in our study were bacteria commonly identified in SSIs: MSSA, methicillin-resistant S. aureus, Acinetobacter baumannii, E. coli, Enterococcus faecalis, P. aeruginosa, and Candida albicans [17,18]. Our results of drain tip cultures and frequencies of SSI-causing pathogens can be used as a reference for empirical antibiotic selection.
The results of bacterial swab cultures performed before and after SSI were compared to investigate the possibility of retrograde infection through drains. Our results demonstrated that the possibility of retrograde infection through drains was higher with open drain placement (55%) than with closed drain placement (41%). In addition, in the open drain group, a sizable proportion of SSI-confirmed patients had their drains removed early, such as on the first or second postoperative day. This indicates that open drains are likely to cause SSI from the beginning of their use. Furthermore, in the closed drain group, though the distribution of SSI occurrence was not high in early drain removal patients, this increased markedly when the drain was removed after 6 days. This demonstrates that even in closed-drain setups, drain insertion sites are susceptible to SSI over time. In addition to these findings from our study, good surgical technique, which includes careful hemostasis, thorough removal of devitalized tissue and foreign bodies, and elimination of dead space at the surgical site, should also be given importance for SSI prevention.
Our study has several unique strengths. First, though many studies have examined SSI risk associated with drains, there were no adequate studies offering insights on controlling and reducing the occurrence of SSIs when drains were used. Our study demonstrates precautionary measures that should be exercised when placing drains to reduce the occurrence of SSIs. Second, based on culture results which were absent in previous studies, we confirmed the differences in causative bacteria behind SSIs and the possibility of retrograde infection according to drain type. Third, against the lack of research assessing the relationship between drain-specific factors and SSI occurrence in plastic surgery patients, our study provided high-quality data from a single center based on follow-up examinations performed by plastic surgeons from the beginning of plastic surgery procedures until the occurrence and resolution of SSI. Finally, by examining the factors known to be related with SSI occurrence from other studies and the distribution of these risk factors in our patients, it was possible to reiterate the importance of these risk factors in reducing the occurrence of SSIs.
However, this study also has some limitations. First, some data were not statistically significant. However, we believe that statistically significant results could be obtained for all parameters with sufficiently increased sample sizes. Second, although we uniformly used a single 2 g intravenous dose of cefazolin within 30 minutes before surgery for preoperative antibiotic prophylaxis, the duration and use of postoperative antibiotics differed depending on wound condition. The effects of postoperative antibiotic use should also have been a consideration of a more thorough study. Moreover, study heterogeneity with respect to multiple types of surgery spread over multiple anatomic locations included in the study was another limitation of our analyses.
In conclusion, the following precautionary measures should be exercised to reduce the occurrence of SSIs when placing drains. First, it is essential to remove drains as early as possible in both open- and closed-drain setups because time to drain removal is a significant risk factor for SSIs. Second, SSIs should be looked out for from the beginning of drain placement when using open drains, considering the high distribution of SSIs among patients with early drain removal and the higher probability of retrograde infection. In closed drains, we recommend removing drains within 6 days after placement. In patients requiring long-term closed drains, clinicians must carefully monitor the characteristics of drain discharge or the wound site status to assess SSI risk. When dressing surgical wounds with drains, any discharge should be pushed outward from the center of the wound to reduce the possibility of retrograde infection in both open and closed drains. Third, consistent with previously reported risk factors for SSI, drains should be withdrawn even earlier in cases of worse wound class. Additionally, smoking cessation and glucose control remain critically important before and after surgery. Nutritional support to adjust malnutrition based on serum albumin levels is also vital to reduce SSIs.
Conflict of InterestYoung Cheon Na is an editorial board member of the journal but was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported. Fig. 1.Drains used in this study. (A) Silicon drain used for open drain placement. (B) Hemovac drains used for closed drain placement (Model No.: PP200L, PP400L). 
Fig. 2.Clinical example of surgical site infection (SSI). SSI defined according to the Centers for Disease Control and Prevention definition of SSI. 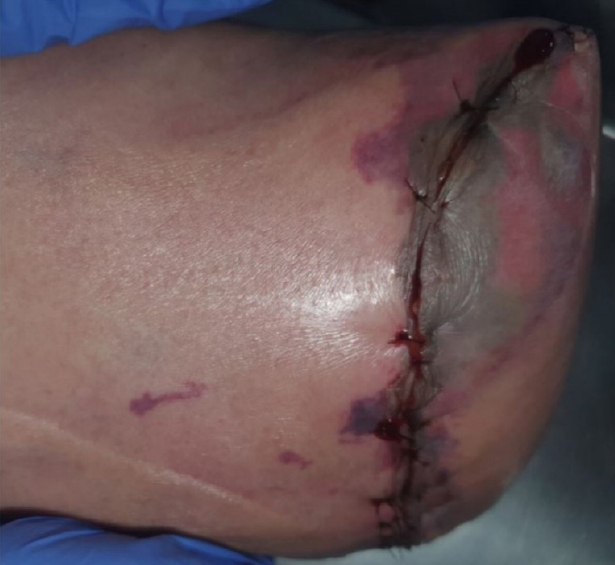
Table 1.Patient distribution according to anatomical site and surgical procedures Table 2.Number of surgical site infection (SSI) cases in our study
Table 3.Patient distribution according to drain characteristics Table 4.Patient distribution according to other known risk factors for surgical site infection (SSI)
Values are presented as mean±standard deviation or number (%). t-tests were performed for age, body mass index, and albumin level. Mann-Whitney test was performed for the duration of surgery. The chi-square test was performed for sex, lifestyle factors (smoking, alcohol consumption), and wound class. Table 5.Patient distribution according to comorbidities associated with surgical site infection (SSI) Table 6.Patient distribution by drain type and time to drain removal
Table 7.Patient distribution according to drain type and wound class Table 8.Distribution of patients with surgical site infection according to time to drain removal time and drain type Table 9.Distribution patients with surgical site infection according to drain type and drain tip culture results References1. Klevens RM, Edwards JR, Richards CL Jr, et al. Estimating health care-associated infections and deaths in U.S hospitals, 2002. Public Health Rep 2007;122:160-6.
2. Mangram AJ, Horan TC, Pearson ML, et al. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol 1999;20:250-78.
3. Owens CD, Stoessel K. Surgical site infections: epidemiology, microbiology and prevention. J Hosp Infect 2008;70 Suppl 2:3-10.
4. Widmer AE, Dangel M. Alcohol-based handrub: evaluation of technique and microbiological efficacy with international infection control professionals. Infect Control Hosp Epidemiol 2004;25:207-9.
5. Drinkwater CJ, Neil MJ. Optimal timing of wound drain removal following total joint arthroplasty. J Arthroplasty 1995;10:185-9.
6. Parker MJ, Livingstone V, Clifton R, et al. Closed suction surgical wound drainage after orthopaedic surgery. Cochrane Database Syst Rev 2007;2007:CD001825.
7. Reiffel AJ, Barie PS, Spector JA. A multi-disciplinary review of the potential association between closed-suction drains and surgical site infection. Surg Infect (Larchmt) 2013;14:244-69.
8. Horan TC, Gaynes RP, Martone WJ, et al. CDC definitions of nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Am J Infect Control 1992;20:271-4.
9. Korol E, Johnston K, Waser N, et al. A systematic review of risk factors associated with surgical site infections among surgical patients. PLoS One 2013;8:e83743.
10. Alfonso-Sanchez JL, Martinez IM, Martin-Moreno JM, et al. Analyzing the risk factors influencing surgical site infections: the site of environmental factors. Can J Surg 2017;60:155-61.
11. Dominioni L, Imperatori A, Rotolo N, et al. Risk factors for surgical infections. Surg Infect (Larchmt) 2006;7 Suppl 2:S9-12.
12. Culver DH, Horan TC, Gaynes RP, et al. Surgical wound infection rates by wound class, operative procedure, and patient risk index. National Nosocomial Infections Surveillance System. Am J Med 1991;91(3B):152S-157S.
13. Mujagic E, Zeindler J, Coslovsky M, et al. The association of surgical drains with surgical site infections: a prospective observational study. Am J Surg 2019;217:17-23.
14. Wilson AP, Gibbons C, Reeves BC, et al. Surgical wound infection as a performance indicator: agreement of common definitions of wound infection in 4773 patients. BMJ 2004;329(7468):720.
15. Howard DD, White CQ, Harden TR, et al. Incidence of surgical site infections postcolorectal resections without preoperative mechanical or antibiotic bowel preparation. Am Surg 2009;75:659-63.
16. Alexander JW, Solomkin JS, Edwards MJ. Updated recommendations for control of surgical site infections. Ann Surg 2011;253:1082-93.
17. Sievert DM, Ricks P, Edwards JR, et al. Antimicrobial-resistant pathogens associated with healthcare-associated infections: summary of data reported to the National Healthcare Safety Network at the Centers for Disease Control and Prevention, 2009-2010. Infect Control Hosp Epidemiol 2013;34:1-14.
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||